If you have ever sat with a stack of curriculum samples on your desk, opened the first one, and thought “this is the same content I read in the last three,” you are not the only person in that chair. Curriculum directors and health coordinators describe the same pattern: every program seems to teach the same topics in roughly the same order. Anatomy. Hygiene. Reproduction. A brief unit on consent. And yet, when these programs are evaluated for outcomes, most produce only modest gains, and many produce no measurable change in student behavior at all.
That gap, between what curricula teach and what students actually do, is the most important variable in your evaluation. It is also the one most programs cannot answer for. A curriculum should tell you, plainly, why it expects to change behavior, not just deliver information. The clearest answer comes from a behavioral science framework called the Health Belief Model, and how a curriculum applies it tells you most of what you need to know.
Why information-only sex education falls short
The original assumption behind a lot of sex education was straightforward. If students learn the facts, they will make better decisions. Decades of research have not been kind to that assumption. Programs that focus primarily on information transfer, the facts of anatomy, reproduction, and risk, consistently underperform programs that build skills. Students may pass the post-test and still struggle to apply the same content in a real conversation, a peer-pressure moment, or a decision point at age 13.
The reason is not that information is unimportant. It is essential. The reason is that knowledge sits at the top of a longer chain. A student needs to know the fact, believe it applies to them, feel capable of acting on it, have the words and behaviors rehearsed enough to use them under pressure, and live in an environment that reinforces healthy choices. A curriculum that stops at the first link in that chain is, in effect, asking students to invent the rest of the chain themselves.
Knowledge sits at the top of a longer chain. A curriculum that stops at the first link is asking students to invent the rest of the chain themselves.
This is the structural reason that strong public support for sex education (84 percent of parents, in repeated surveys) coexists with student outcome data that has been stuck for years. The support is there. The framework many curricula use is incomplete.
What the Health Belief Model actually says
The Health Belief Model is one of the most-studied behavior change frameworks in public health. It was developed in the 1950s to understand why people did or did not adopt health behaviors, and it has been adapted across smoking cessation, HIV prevention, cancer screening, vaccination, and dozens of other contexts. The version used in PWY is an adaptation specifically for school-based puberty and sex education, and it identifies four factors that all need to be present before a student can be expected to act on what they have learned.
The four factors are:
- Knowledge. Accurate, age-appropriate information about puberty, anatomy, relationships, and sexual health.
- Self-efficacy. The student’s confidence that they can use this information in their own life. A sense of personal vulnerability balanced with a sense of personal control.
- Skills. Practiced and rehearsed abilities, especially communication, refusal, decision-making, and help-seeking. The practiced part matters.
- Environmental support. Reinforcement from families, teachers, and community that supports the healthy choice.

A program targeting only Factor 1 cannot produce reliable behavior change, because the chain breaks at Factor 2 or 3. A program targeting all four does not guarantee behavior change either. Schools cannot fully control a student’s home environment or their peer group. But it builds the conditions under which behavior change becomes likely, observable, and measurable.
This is the question worth asking of every curriculum on your desk. Which of the four factors is this curriculum building, and how does it know?
How the four factors look in a real curriculum
In practice, a curriculum built on the adapted Health Belief Model treats every lesson as targeting more than one factor. Lessons do not split into “knowledge lessons” and “skills lessons.” A single lesson on healthy relationships, for example, is expected to do four things at once.
It teaches the relevant knowledge: what makes a relationship healthy, what does not. It builds self-efficacy by helping students identify what they already do well and where they can grow. It teaches a skill (communicating a need, listening to a partner, recognizing a boundary violation) using a defined four-step instructional process. And it activates environmental support, often through a Family Activity Sheet that brings the conversation home with a parent or trusted adult, then back to school the following week.
Audit prompt for your selection committee: Pick a single lesson from any curriculum on your desk. Can you trace where it builds knowledge, self-efficacy, skills, and environmental support? If two of the four are missing, the lesson is unlikely to change behavior, no matter how strong the content is.
When a curriculum is structured this way, you can audit a single lesson and see whether all four factors are present. You can also predict what evaluation results will look like. If a curriculum reports knowledge gains but no behavior change, that is consistent with a curriculum targeting Factor 1 only. If it reports gains in self-reported confidence, communication skill demonstrations, and home conversation rates, that is consistent with a curriculum targeting all four.
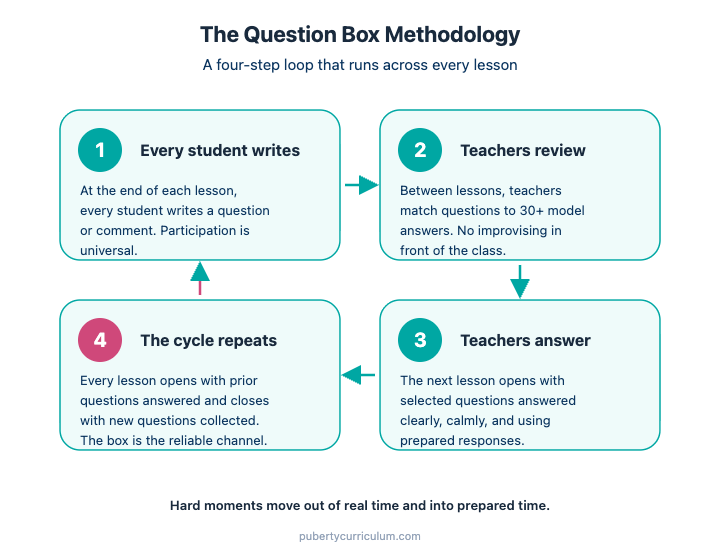
PWY is built around this structure. Every grade-level unit in the grades 4-6 sequence applies the model, and every lesson within those units is designed to move students through more than one factor. The Skills-Based Instruction 4-step model (explain and motivate, model and demonstrate, practice with feedback, apply to real-life situations) is the practical engine that builds Factor 3 inside every skill lesson. The Family Activity Sheets and Family Partnership Flyers are the primary mechanism for Factor 4. The Question Box methodology, in which every student writes every lesson, supports both Factor 1 and Factor 2, because students learn that their real questions are taken seriously and their concerns are not unique.
What this means for your curriculum evaluation
For a curriculum director evaluating options, the Health Belief Model gives you a sharper lens than a topic checklist. State frameworks tell you what topics must be covered. They tell you very little about whether the curriculum can actually move students toward healthier behavior. The model lets you ask deeper questions of any program.

Five questions to bring into your evaluation:
- Does this curriculum name the behavioral science framework it is built on? A curriculum that cannot articulate why it expects to work is unlikely to produce reliable results across teachers and classrooms.
- Does each lesson target more than one factor? Or is the curriculum structured as a knowledge sequence with skills bolted on at the end?
- What is the instructional process for teaching a skill? A defined, repeatable model (such as the 4-step explain-model-practice-apply pattern) makes fidelity evaluation straightforward and supports teachers of all experience levels.
- How does the curriculum activate the home environment? A line in the appendix is not the same as a Family Activity Sheet that brings the conversation home as a structured assignment.
- What evaluation data exists, and what does it measure? Knowledge gains alone tell you Factor 1 worked. Look for outcomes across self-efficacy, demonstrated skill, and home reinforcement.
Curriculum directors who use this lens regularly report that the conversation with a selection committee shifts. Instead of comparing programs feature-by-feature, the committee can ask one question of every program: how is this curriculum going to change behavior, and how will we know? That is a question most committees can answer together, even when they disagree on tone or emphasis.
A defensible foundation, not a brand label
The Health Belief Model is not a PWY invention. It is a public health framework with decades of research behind it, applied across many domains, including sex and relationships education. What PWY contributes is a specific, school-tested adaptation of the model built into a curriculum for grades 4 through 6, paired with named instructional methods (Skills-Based Instruction, the Question Box methodology, the “Freedom To” philosophy, trauma-informed design) that operationalize the model in a classroom.
This is the foundation on which the rest of the curriculum sits. It is also the answer to the most common question a curriculum director eventually has to defend in a board meeting: why should we expect this program to produce different results than the one we are using now? The answer comes back to the framework. Targeting four factors at once, with an instructional design consistent enough that any teacher who follows the script can deliver the model with fidelity, is what produces measurable, defensible outcomes. That is true of PWY, and it is the standard worth holding any curriculum to.
If you are in an active adoption window or evaluating options for the next school year, the next step is to look at how a curriculum applies these four factors in a real lesson. PWY offers a free 60-day curriculum preview for districts evaluating their next program, so your selection committee can see the framework in action across grades 4, 5, and 6. Two posts worth reading alongside the preview are PWY’s curriculum evaluation framework and the recent piece on positive versus fear-based puberty education, which together cover the evaluation criteria most curriculum directors find useful in committee conversations.
Knowledge alone does not change behavior. The curriculum that recognizes that, in its design, is the curriculum worth bringing to your selection committee.